CORNEA TRANSPLANTS
A cornea transplant is a surgical procedure that replaces diseased or scarred corneal tissue with healthy tissue from an organ donor.
There are two main types of cornea transplants: traditional, full thickness cornea transplant (also known as penetrating keratoplasty, or PK) and partial thickness cornea transplant (referred to as endothelial keratoplasty, or EK).
A donor corneal graft replaces central corneal tissue, damaged due to disease or eye injury, with healthy corneal tissue obtained from a local eye bank. An unhealthy cornea affects your vision by scattering or distorting light and causing glare and blurred vision. A cornea transplant may be necessary to restore your functional vision.
Corneal eye disease is the fourth most common cause of blindness (after cataracts, glaucoma and age-related macular degeneration) and affects more than 10 million people worldwide.*
More than 44,000 cornea transplants are performed in the United States each year, according to an estimation by the Eye Bank Association of America.
WHEN DO YOU NEED A CORNEA TRANSPLANT?
A healthy, clear cornea is essential for good vision. If your cornea is damaged due to eye disease or eye injury, it can become swollen, scarred or severely misshapen and distort your vision. When less invasive medical treatment fails, a corneal transplant may be the only remaining option.
A corneal transplant is commonly performed for the following conditions:
- Eye diseases such as advanced Keratoconus
- Scarring from infections, such as herpes or fungal keratitis.
- Hereditary conditions such as Fuchs’ dystrophy.
- Chemical burns of the cornea or damage from an eye injury.
- Excessive swelling (edema) of the cornea.
- Graft rejection following a previous corneal transplant.
- Corneal failure due to cataract surgery complications.
- Rare complications from LASIK surgery.
ARE YOU A CORNEA TRANSPLANT CANDIDATE?
A cornea transplant is performed to improve vision. If pain is caused by a significantly diseased or damaged cornea, a cornea transplant may relieve that symptom.
With these factors in mind, you also should consider several important questions before you decide to undergo a corneal transplant:
- Does your functional vision impede your job performance or your ability to carry out daily activities?
- Can your vision be corrected with special or other less invasive measures?
- How will the cost of cornea transplant surgery affect your financial situation if your insurance does not cover everything from pre-screening to post-operative consultations?
- Are you able to take enough time off from work or school (up to six months to a year in some cases) to recover properly?
All of these questions, in conjunction with a thorough screening and consultation with your eye doctor, must be carefully considered before you make the final decision to have a corneal transplant.
BEFORE THE PROCEDURE
Before a donor cornea is released for use in transplant surgery, it is checked for clarity and screened for the presence of any diseases such as hepatitis, HIV and many other infections, in accordance with the Eye Bank Association of America’s strict medical standards and FDA regulations. Only corneas that meet these stringent guidelines are used in corneal transplant surgery to ensure the health and safety of the graft recipient.
DURING THE CORNEA TRANSPLANT
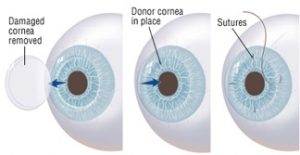
Traditional corneal transplant surgery. During traditional corneal transplant surgery, or penetrating keratoplasty (PK), a circular button-shaped, full-thickness section of tissue is removed from the diseased or injured cornea . A matching “button” from the donor tissue is then positioned and sutured into place. The sutures (stitches) remain in place typically for a year or more after surgery.
Lastly, a plastic shield is placed over your eye to protect it during healing.
Penetrating keratoplasty surgery generally takes one to two hours and most procedures are performed on an outpatient basis, meaning you can go home a short while after the surgery (though you will need someone to drive you home).
Endothelial keratoplasty. In 2003, a newer version of corneal transplant surgery called endothelial keratoplasty (EK) was introduced for certain corneal conditions.
Endothelial keratoplasty selectively replaces only the innermost layer of the cornea (endothelium) and leaves the overlying healthy corneal tissue intact. The endothelium controls the fluid balance in the cornea, and if it becomes damaged or diseased, this can cause significant corneal swelling and loss of vision.
In EK, the surgeon makes a tiny incision and places a thin disc of donor tissue containing a healthy endothelial cell layer on the back surface of your cornea. An air bubble is used to position the new endothelial layer into place. The small incision is self-sealing and typically no sutures are required.
Endothelial keratoplasty has several advantages over full-thickness penetrating keratoplasty. These include: faster recovery of vision; less operating time; minimal removal of corneal tissue (and therefore less impact on the structural integrity of the eye and less susceptibility to injury); no related suture complications; and reduced risk of astigmatism after surgery.
Within a relatively short period of time, the EK corneal graft procedure has become the preferred technique for patients with Fuchs’ dystrophy and other endothelial disorders of the cornea. However, traditional full-thickness PK is still the most appropriate option when the majority of your cornea is diseased or scarred.
RECOVERING FROM A CORNEA TRANSPLANT
Total recovery depends upon the type of corneal transplant and can vary from a few months up to a year, or longer.. Initially, your vision will be blurry for the first few months — and in some cases may be worse than it was before — while your eye gets used to its new cornea.
As your vision improves, you will gradually be able to return to your normal daily activities. For the first several weeks, heavy exercise and lifting are prohibited. Your doctor will also recommend a timeline specific to you for returning to work, school or resuming other activities.
Steroid eye drops will be prescribed for several months to help your body accept the new corneal graft, as well as other medications to help control infection, discomfort and swelling. You should keep your eye protected at all times by wearing a shield or a pair of eyeglasses so that nothing inadvertently bumps or enters your eye.
If stitches were used in your surgery, they usually are removed six months to a year post-surgery, depending on the health of your eye and the rate of healing. Adjustments can be made to the sutures surrounding the new corneal tissue to help reduce the amount of astigmatism resulting from an irregular eye surface.
As with any type of surgery, always follow the instructions of your eye surgeon to help minimize corneal transplant complications and expedite healing.
CORNEA GRAFT REJECTION
Cornea transplants are performed routinely and have a reasonable success rate. In fact, cornea grafts are the most successful of all tissue transplants.
Cornea transplant rejection can be reversed in 9 out of 10 cases if detected early enough.
Like any other surgical procedure, a cornea transplant comes with certain risks. But, for most people, having their vision improved or restored outweighs the potential complications associated with cornea transplant surgery. It is a very personal decision for a patient to decide to undergo cornea transplant surgery.
Complications of a corneal transplant can be significant and can include cornea graft rejection, eye infection and problems associated with the use of stitches.
Rejection of the donor tissue is the most serious complication after a corneal transplant and occurs in five to 30 percent of patients. Transplant rejection is when your body’s immune system detects the donor cornea as a foreign body and attacks and tries to destroy it.
Recognizing the main warning signs of corneal transplant rejection is the first step to preventing graft failure. These can be remembered using the acronym RSVP:
- Redness
- Extreme Sensitivity to light
- Decreased Vision
- Pain
Rejection signs may occur as early as one month or as late as several years after surgery. Your eye doctor will prescribe medication that can help reverse the rejection process. If detected early, the graft will be successful 9 out of 10 times, according to the Cornea Research Foundation of America.
Should your graft fail, corneal transplant surgery can be repeated. While repeat surgery generally has good outcomes, overall rejection rates increase with the number of corneal transplants you have.
VISION AFTER A CORNEA TRANSPLANT
Your eyesight should gradually improve a few weeks after a corneal graft, but it could take anywhere from a couple of months up to a year to have stable vision in the eye that receives the donor tissue.
Because your vision will fluctuate during the first few months following your surgery, it is advisable to wait until your eye doctor tells you your vision is stable before you fill an eyeglass prescription or are fitted for contact lenses.
After your eye has fully healed and any stitches used have been removed, you may be eligible to undergo laser eye surgery such as LASIK or PRK to improve your ability to see with or without glasses or contacts by reducing myopia and astigmatism.





